Chronic Cystitis
Chronic cystitis is a general term used to describe various types of inflammatory conditions of the bladder. In this article I will describe the methods of determining the correct diagnosis and successful treatment.
Diagnosis: chronic cystitis
Specifics: if we think about it, it turns out that there are many different types of cystitis such as bacterial recurrent cystitis, fungal and viral cystitis, chronic pelvic pain syndrome, cystitis after intercourse and leukoplakia of the bladder. The causes and types of bladder inflammation are numerous but “chronic cystitis” is not among them. It is simply a general term for a number of different types of “cystitis”, each of them treatable given the detailed diagnosis and removal of the factors causing the inflammation of the bladder.
What are we treating? The general term? It is not treatable as it simply does not exist. Are we removing the pain? It is not treatment, it’s simply wishful thinking. Treatment of chronic cystitis depends entirely on the cause.
Treatment of Chronic Cystitis
- Identifying and removing the focal point of infection in chronic cystitis is the first task for the doctor.
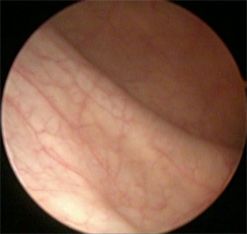
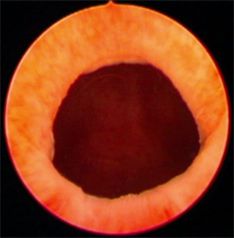
- Cystoscopy under anaesthetic – essential investigation allowing us to pinpoint the cause or to determine that the bladder is healthy.
- Bladder mucosa biopsy – allows us to get a detailed histological diagnosis. This procedure is carried out during cystoscopy.
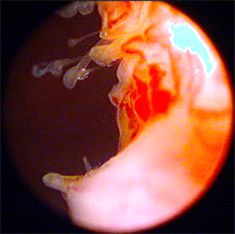
- Bladder instillation – is administration of medication into the bladder with the aim of normalising the condition of the bladder mucosa.
- Vaporization treatment of leukoplakia – in cases where leukoplakia is detected and identified to be the cause of “chronic cystitis”.
“Doctor, I suffer from chronic cystitis”; “Constant pelvic pain, I am drinking 2 liters of water a day and get terrible water retention as a result but if I stop drinking the pain is unbearable”; “Bladder inflammation comes and goes after giving birth”; “I cannot live a normal life, as soon as I get slightly chilled it all starts. I am reluctant to leave the house and go outside”; “I have visited all of the specialists: The urologist refers me to a gynaecologist, the gynaecologist prescribes antibiotics, cystitis goes away briefly and comes back again”.

All of the above are typical complaints of my female patients suffering from “chronic cystitis”. Each one of them has a very thick folder of medical notes and each one of them has their life ruined by cystitis and every single one of them has a verdict diagnosis of: “Chronic cystitis”. Countless tests and investigations, “immune system strengthening” and homeopathy all provide a very short lived relief and then it gets worse again. I will clarify that in this section we are talking about bladder inflammation and not about chronic pelvic pain. With the latter the urine tests often do not show anything, cystoscopy may not detect any changes and the bladder appears completely healthy. This condition will be discussed in the section “Chronic pelvic pain in females”.
So what is chronic cystitis?
Usually the “chronic cystitis diagnosis” means that the patient has tried many antibacterial medication treatments, is familiar with the term “immune response modifier” and is taking prebiotics to treat the mystical illness under the name of “bacterial imbalance”. In other words I see before me a woman that no longer even believes that she can be cured. And the reason is incorrect diagnosis. Just think….if we call a condition “chronic cystitis” we must cure it chronically, i.e constantly and with something that gets rid of the inflammation. Logically antibiotics are the correct treatment. So why do they not help? The bacteria identified in the urine were sensitive to antibiotics. Why then after about 7 days of completing the treatment cystitis returns? Why if a woman has a glass of wine, eats something spicy or takes a longer walk in the park does the cystitis comes back and stay longer this time?
The answer is simple: “chronic cystitis” is always caused by some other condition. It is either the source of bacteria from which they can constantly get into the bladder or there is an underlying pathology of the bladder or the urethra making it easier for the bacteria to get into the bladder and stick to the bladder mucosa while multiplying, or there could be both the source of bacteria and bladder pathology present.
Causes of chronic cystitis
It is very important to understand that true leukoplakia is a very rare and supposedly pre-cancerous change in the mucosa. It has nothing to do with chronic cystitis. And in this article as well as in other publications the term “Leukopakia of the bladder” refers to “vaginal mucosa metaplasia”. It is simply an incorrect term which has now established itself in medical terminology. True leukoplakia does not develop under the influence of ureaplasma, chlamydia and viruses. All of these are more likely to be the cause of vaginal metaplasia. Millions of women have a “leukoplakia” diagnosis and do not have a pre-cancerous bladder condition. This is because they do not suffer from the true leukoplakia but from vaginal metaplasia which causes benign changes in the bladder mucosa
which in some cases causes symptoms such as pain and burning sensation in the pelvic area.
True leukoplakia is a very rare pathological condition. The term leukoplakia is used here to describe “vaginal metaplasia” which manifests as changes in the mucosa following inflammation.
Symptoms of chronic cystitis
In all cases the woman feels the urge to empty the bladder frequently, there can be flare ups of acute cystitis, the feeling of heaviness and discomfort in the bladder. Sometimes there can be blood in the urine. The patient has to take numerous painkillers, is prescribed antibiotics and seemingly overcomes the infection. But she already knows that chronic cystitis will be back.

—Hello, please come in and take a seat. How can I help?
— I suffer from chronic cystitis
— And what are your symptoms? — I ask this question as cystitis can cause a great number of symptoms and I need to make sure that it is truly cystitis and not urethritis for example.
— Well, you know, I had a cold a few years ago and had acute cystitis as a result. I took the medication prescribed but it did not completely go away, the discomfort in the pelvic area remained accompanied by pain and the urge to go to the toilet frequently. It seems to get better if I drink plenty of fluids. But if I get the slightest cold it seems I never leave the toilet, I keep getting tests and sometimes e-coli is present and sometimes not. How can I get rid of it? I have tried all available antibiotics.
I look at her numerous tests results. Urine tests, blood tests, smear tests. Some time ago a ureaplasma and chlamydia diagnosis was made and both were thoroughly treated with antibiotics. Now the smear tests are normal. She was also previously diagnosed with human papilloma virus but all is clear now.
I examine the patient in the chair. Nothing remarkable. The urethra is positioned normally and peri-urethral glands are not tender. No other pathology is visible. I perform a kidney ultrasound and again there is nothing. No tumours or kidney stones. The neck of the bladder is slightly thickened.
— Have you had a cystoscopy?
— No, doctor, I am too afraid. It is supposedly very painful according to the information on all the forums. And they never find anything..
— Cystoscopy is essential. It is important to see what is going on with the bladder mucosa. I guarantee that it will not be painful, we will carry it out under anaesthetic.
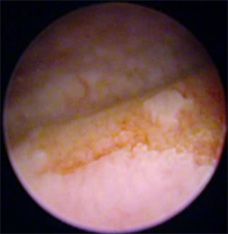
A few days later cystoscopy and biopsy of the bladder was performed. Severe leukoplakia was detected in the neck of the bladder and small polyps in the urethra.
Professor Z Weinberg
Chronic cystitis diagnosis
So what is the story with our patient? Some time ago, after suffering from acute cystitis as well as ureaplasma and chlamydia infection she developed leukoplakia of the neck of the bladder (to be exact her histology report said “vaginal metaplasia”). In addition small polyps in the urethra were present.
Leukoplakia of the bladder or vaginal metaplasia is the replacement of the transitional epithelium of the bladder with flat squamous epithelium cells.
What hides behind this mysterious term? Why does replacing one kind of epithelium with another lead to constant pain, discomfort and urges to go to the bathroom? Here is the thing. Healthy mucosa isolates and protects the underlying bladder wall containing sensitive nerve endings from the effects of urine. When inflammation, STDs, viruses or endocrine problems lead to leukoplakia this defence is broken. The urine starts penetrating the underlying wall thus irritating the nerve endings and causing constant discomfort, pain and the urge to urinate. According to various data sources up to 63% of women complaining of the above symptoms suffer from bladder leukoplakia.
And here we have a catch 22, or even several. Acute cystitis always leads to treatment with antibiotics. But acute cystitis is at the same time the manifestation of leukoplakia which leads to…yet another flare up of acute cystitis. Should one really be surprised that the patient knows the names of all available antibiotics and is very familiar with procedures such as iontophoresis, bladder infusions and homeopathy. And all of those without any visible affect…. But she does have Chronic! Cystitis after all.
Wrong. She does not have chronic cystitis. Her diagnosis is as follows: “Leukoplakia (or vaginal mataplasia) of the neck of the bladder. Urethral polyps. Chronic recurrent bacterial cystitis.” Can these be cured? Of course. Leukoplakia of the bladder and the urethral polyps can be treated. And by removing the cause we will give back to the person their quality of life without constant worry anticipation of yet another chronic cystitis flareup.
Treatment of Chronic Cystitis
Treatment of Chronic Cystitis is first and foremost the identification and removal of the cause. Is it possible to treat a vague and unclear diagnosis? Doubtful. But is it possible to treat Leucoplakia of the bladder neck? Yes, it is. How about the urethral polyps? Definitely. Bladder stone? Without any doubt. Deep positioning of the urethra causing cystitis after intercourse? Of course.
Thus, the correct treatment of chronic cystitis is only possible with detailed diagnosis. For example, what does the diagnosis of “Vaginal urethral dystopia with chronic recurrent post-coital cystitis” tell us? It tells us that the cause of cystitis is the incorrect positioning of the urethra and that during intercourse the urethra gapes and the penis pumps bacteria into the bladder. Is it possible to treat this form of chronic cystitis? Yes, without doubt. But because the treatment of chronic cystitis is not possible without the detailed diagnosis I do not recommend trying to treat chronic cystitis yourself. Just think, only a consultation with a patient and examination takes around 30 or 40 minutes. Gynaecological examination is also necessary to assess the condition of the urethra and vaginal mucosa. As well as an ultrasound of the kidneys, renal ducts and the bladder. Cystoscopy should be carried out with the use of anaesthetic as the patient should not be feeling the pain. Sometimes we need to perform general and detailed urography, functional tests such as urodynamic study. Urine tests are also always carried out. All the results require correct interpretation. There is an opinion that a doctor identifying the diagnosis as “chronic cystitis” is them admitting the fact that they have not got to the bottom of the cause...
Modern treatment of chronic cystitis has three goals: removal of the external cause of cystitis, fighting the existing infection and restoration of the bladder mucosa.

... — I recommend surgery. We need to remove the polyps and leukoplakia of the bladder.
— Surgery? You are going to cut?!
— Hmm. Let’s say it’s a surgery without the cuts. Transurethral resection of leukoplakia and the polyps. It is carried out through the urethra with the help of endoscopy.
— It is very frightening. Will I have to stay in hospital long? Is it painful?
— No. It won’t hurt. The surgery is performed under spinal or intravenous anaesthesia, you chose. After the surgery you will need painkillers for 1 or 2 days. The day following the operation I can discharge you to go home and you can go to work the next day after that. I followed up this patient for 18 months after her surgery. She got married and had a healthy baby. She forgot she ever had chronic pain, cystitis flareups and had to constantly take antibiotics.
If you require diagnosis and treatment of chronic cystitis in Moscow please contact us. We will arrange and carry out all the necessary tests, establish the diagnosis and provide a treatment plan. You will be able to return home after 1 day.