Varicocele
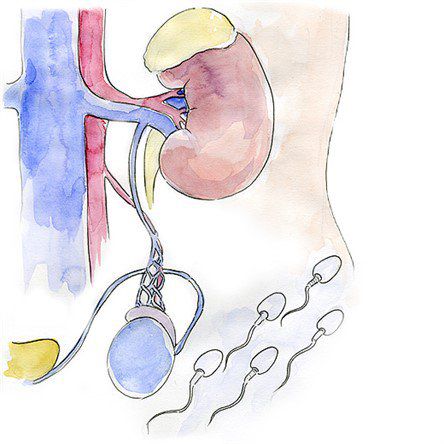
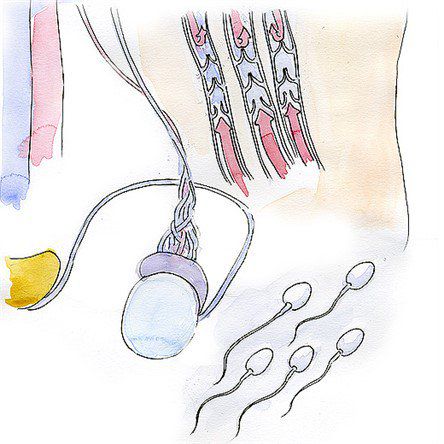
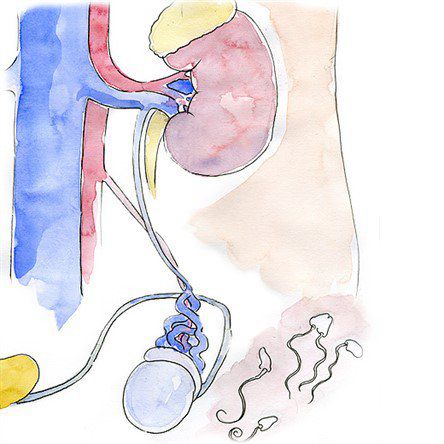
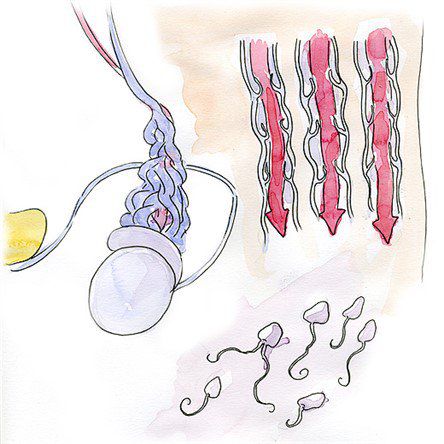
Varicocele is a condition seen in men and adolescent boys, which manifests as varicose veins in the testicles and spermatic cord. Up to 40% of male infertility can be attributed to this condition. In this article I will explain the reasons and the consequences of varicose veins in the testicles and go over the treatment methods.